When was your last eye exam? If you’re unsure, you’re not alone. Many people delay scheduling an appointment until they notice changes in their vision. However, routine comprehensive eye exams are essential for maintaining optimal eye health, detecting problems early, and preserving clear vision throughout every stage of life. Understanding how often to visit an eye doctor can help you stay proactive about your health and prevent potential complications.

What Is a Comprehensive Eye Exam?
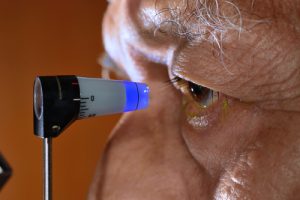
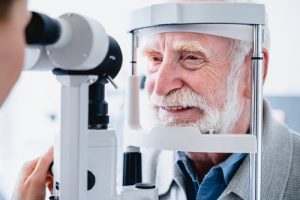
A comprehensive eye exam goes far beyond a basic vision screening. While screenings simply measure how well you see, a full examination evaluates both your visual acuity and the overall health of your eyes. During the appointment, an ophthalmologist assesses your prescription, eye coordination, and internal eye structures such as the retina and optic nerve.
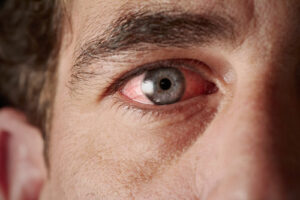
Using advanced diagnostic technology, comprehensive exams can detect early signs of conditions like cataracts, glaucoma, macular degeneration, and diabetic retinopathy—often before noticeable symptoms develop. These thorough evaluations play a critical role in preventing vision loss and ensuring long-term eye health.
How Often Should You Schedule an Eye Exam?
The ideal frequency for comprehensive eye exams depends on your age, lifestyle, and medical history. While individual needs may vary, general guidelines include:
- Children and Teenagers: Every 1–2 years to support proper vision development and academic success.
- Adults Ages 18–39: Every 2 years if no vision problems or risk factors are present.
- Adults Ages 40–64: Every 1–2 years as age-related changes and eye disease risks increase.
- Adults Ages 65 and Older: Annually to monitor for conditions such as cataracts, glaucoma, and macular degeneration.
- High-Risk Individuals: More frequent exams may be necessary for those with diabetes, high blood pressure, a family history of eye disease, or existing vision concerns.
An ophthalmologist can recommend a personalized schedule based on your specific needs.
Why Regular Eye Exams Matter
Routine eye exams are about more than just updating your glasses or contact lens prescription. Many serious eye conditions develop gradually and without symptoms, making early detection essential. Comprehensive exams allow for timely treatment, reducing the risk of permanent vision loss.
In addition to safeguarding your eyesight, eye exams can reveal signs of broader health concerns such as diabetes, hypertension, and high cholesterol. Because the eyes provide a unique view of blood vessels and nerves, they often serve as an early indicator of systemic conditions.

Advanced Eye Care You Can Trust
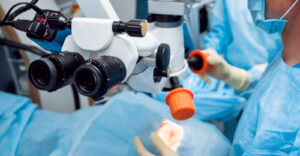
Patients seeking expert care can rely on Sierra Nevada Eye Center. Specializing in ocular surgery and the treatment of ophthalmic disorders, the practice utilizes state-of-the-art technology to deliver exceptional patient care. With facilities in Reno, Renown, and Carson City, their experienced team provides comprehensive eye exams and advanced treatments tailored to each individual.
Protect Your Vision for the Future
So, how often should you get a comprehensive eye exam? The answer depends on your age, health, and risk factors—but regular visits are essential for preserving lifelong vision. By prioritizing routine eye care, you can detect issues early, maintain clear sight, and protect your overall well-being.
If it’s been a while since your last exam, now is the perfect time to schedule one, or give us a call, and take a proactive step toward healthier vision.