
Glaucoma is often called “the silent thief of sight” as it can steal your vision without you even knowing it. Glaucoma is the leading cause of blindness in the United States. The progression of the disease is very slow, so you may not even notice the changes in your vision before irreversible damage has already occurred. This can be prevented. Sierra Nevada Eye Center recommends regular eye examinations to detect and treat early symptoms of glaucoma as well as other potential eye problems.
Sierra Nevada Eye Center provides expertise in the diagnosis and management of glaucoma. Dr. Robert Wolff and Dr. Michael Westafer have extensive experience in glaucoma care and surgery. As a fellowship-trained glaucoma specialist, Dr. Westafer specializes in the treatment of all forms of glaucoma. Click here or call to schedule an appointment with the best glaucoma specialists in Nevada.
What is glaucoma?
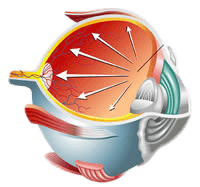
Glaucoma is an eye disease that damages the optic nerve (which connects the back of the eye to the brain), often associated with high pressure in the eye. There are many different types of glaucoma; the two basic types of glaucoma are primary open angle glaucoma (POAG) and angle-closure glaucoma. POAG is the most common type; the cause of POAG is not yet known, and there is no cure.
What are the symptoms of glaucoma?
POAG is usually chronic and painless; angle-closure glaucoma may develop rapidly and result in eye pain. And because glaucoma damages the peripheral vision first, most patients do not know they have POAG until they are checked by an eye doctor. As glaucoma damage to the optic nerve progresses, loss of peripheral vision leads to tunnel vision, then blindness. Glaucoma damage is permanent and cannot be reversed.
How is glaucoma diagnosed?
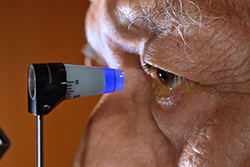
Glaucoma is detectable with an eye exam and special testing. Evaluation includes measurement of vision, intraocular pressure (IOP), corneal thickness, gonioscopy (to check the drainage tissue in the eye), and optic nerve function. We use the most advanced technology and equipment to assess optic nerve function, including visual field testing to check peripheral vision damage, and optical coherence tomography (OCT) to evaluate optic nerve tissue damage. Since there can be a genetic component to glaucoma, family members may need to be tested as well.
How is glaucoma treated?

Though there is no cure for most cases of glaucoma, it can be controlled by lowering the intraocular pressure (IOP) to a safe level. Most commonly, a laser procedure (SLT) or eye drops are used lower IOP. The drops work by either reducing the production of aqueous (fluid in the front chamber of the eye) or increasing drainage of aqueous out of the eye. In some types of glaucoma, a laser procedure may be required initially. When eye drops do not control IOP adequately, glaucoma laser or surgery may be necessary. Treatment and monitoring of glaucoma is continued life-long to ensure that progressive optic nerve damage does not occur. It is extremely important for glaucoma patients to keep taking their eye drops regularly, and to follow-up with the eye doctor as instructed.
What is glaucoma laser?
There are several types of glaucoma laser procedures:
Laser Trabeculoplasty – the trabecular meshwork (the drainage tissue inside the eye) is treated to allow aqueous to drain out of the eye more easily. This is a quick procedure performed in the office or outpatient
surgery center. Most commonly, selective laser trabeculoplasty (SLT) is performed.
Laser Iridotomy – an opening is made in the iris to create an alternate pathway for aqueous to circulate. This is used for narrow angle or angle closure glaucoma. This is a quick procedure performed in the office or outpatient surgery center.
Endocyclophotocoagulation (ECP) – the ciliary body tissue (which makes aqueous) is treated to decrease production of aqueous. This is performed in an outpatient surgery center, often combined with cataract surgery.
Transscleral Cyclophotocoagulation (CPC) – Laser energy is applied to the sclera, the outer white wall of the eye, thus altering the cells that form fluid inside the eye. As a result, eye pressure is lowered, glaucoma is controlled, and the need for future medical treatment is reduced. This laser procedure is administered in an outpatient surgery center.
Direct Selective Laser Trabeculoplasty (DSLT)
Direct Selective Laser Trabeculoplasty (DSLT) is a non-invasive, automated, first-line glaucoma treatment that aims to lower intraocular pressure (IOP) by directly targeting the eye’s natural drainage system.
Unlike traditional laser procedures, DSLT delivers a fully automated, standardized treatment in seconds with no incisions, minimal discomfort, and no recovery time required. It may help patients reduce or even eliminate the need for daily eye drops, either as an early treatment option or alongside other glaucoma care.
Ask your doctor at Sierra Nevada Eye Center if DSLT is right for you.
What is glaucoma surgery?
The goal of glaucoma surgery is to improve drainage of aqueous fluid to reduce eye pressure. There are a number of different procedures available, such as trabeculectomy, ExPress mini-tube shunt, Ahmed and Baerveldt tube shunts. Dr. Wolff and Dr. Westafer have experience with all of these glaucoma procedures. These procedures drain aqueous fluid directly out of the eye to control glaucoma.
The most common procedure is trabeculectomy, which involves making an opening into the front chamber of the eye to allow aqueous to drain directly out of the eye. A more recent version of trabeculectomy is the ExPress Shunt procedure, which involves using a special tiny tube to drain aqueous from the eye; our Doctors have the most extensive experience with the ExPress Shunt in northern Nevada.
A more recent FDA-approved procedure is canaloplasty. In this procedure, a suture is threaded through Schlemm’s canal (a circular tube that normally drains aqueous fluid from the eye) and tightened, thereby distending Schlemm’s canal to allow increased drainage of aqueous fluid out of the eye, resulting in reduced eye pressure. A significant advantage of this procedure is that it reduces the serious risks and complications that are seen with other glaucoma procedures.
WHAT IS MICRO INCISIONAL GLAUCOMA SURGERY?
MIGS is a group of surgeries that are designed to lower eye pressure for individuals who have glaucoma, all with fewer possible complications. Traditional glaucoma surgeries, such as a trabeculectomy or external tube shunts, can lead to complications such as discomfort, abnormally low eye pressure, and eye infections. Our surgeons have some of the most extensive experience with MIGS in Nevada, including iStent Inject, Hydrus microstent, OMNI, GATT, and Kahook Dual-Blade. Learn more.
For more information about glaucoma, visit the following website:
The Glaucoma Foundation and The Glaucoma Research Foundation.




